The incredibles benefits of breastfeeding
Table of contents
Why Breastfeeding: A Look at the 5 Main Benefits
- 5 main benefits about breastfeeding
- Benefits of breastfeeding for your baby
- Benefits of breastfeeding for you, mom
- The biology behind breastfeeding
- What to do before your baby is born
- Breastfeeding on the practice
- Latching
- What if I cannot breastfeed? Formula
- What to eat while breastfeeding
- Which medication is safe
5 main benefits of breastfeeding
- For the majority of newborns, breast milk is the best source of nutrients. The mother’s breast milk will vary as the infant develops to satisfy his or her nutritional demands.
- Babies who are breastfed may be more resistant to several short- and long-term illnesses and disorders. Breastfed newborns have a decreased incidence of asthma, obesity, type 1 diabetes, and sudden infant death syndrome (SIDS). Babies who are breastfed are also less likely to get stomach illnesses and ear infections.
- Antibodies from the mother are passed on to the infant through breast milk. These antibodies aid in the immune system development of infants and shield them against disease.
- Wherever and at any moment, mothers can breastfeed. Without having to prepare bottles or mix formula, mothers can feed their infants on the move. Breastfeeding while traveling can also be a source of comfort for infants whose regular schedule is disturbed.
- The mother’s health also benefits from breastfeeding. The risk of breast and ovarian cancer, type 2 diabetes, and high blood pressure in mothers can be decreased by breastfeeding.
Benefits of breastfeeding for your baby
Breastfeeding prevents illness
With time, your body will adjust the milk you make to your baby’s needs. In fact, it’s thought that your body receives a “status report” from your baby’s saliva that helps it adjust the amount of nutrients and antibodies in your milk to accommodate your baby’s changing nutritional requirements.
In addition, your body makes antibodies to fight the illnesses you are exposed to, therefore your milk is specially formulated to combat the illnesses your baby is exposed to as well. It is like a natural vaccine.
The American Academy of Pediatrics (AAP) states that breastfeeding can lower your baby’s risk of getting the following diseases and conditions:
- Asthma
- Diarrhea/vomiting
- Respiratory tract infections
- Necrotizing enterocolitis
- Ear infections
- Urinary tract infections
- Late-onset sepsis in preterm infants
- Type 1 and 2 diabetes
- Lymphoma, leukemia and Hodgkin’s disease
- Childhood obesity
- Sudden infant death syndrome
- Bacteremia (the presence of bacteria in the blood)
Breastfeeding helps the digestive tract development
Formulas might be hard for your child’s growing digestive system since they are made from cow’s milk. Your baby’s tummy will need some time to become used to digesting non-human milk. Premature newborns are most affected by this.
Contrarily, breast milk contributes to the bifidobacteria lining your infant’s digestive system, which is beneficial bacteria that can inhibit the formation of dangerous organisms. Moreover, breast milk is always sterile since it is produced straight from the breast. This guards against stomach problems like diarrhea.
Breastfeeding helps jaw musculature to form correctly
While it is more difficult for your infant to acquire milk from your breast than a bottle, breastfeeding encourages jaw growth. Breastfeeding strengthens your baby’s jaw and promotes the development of straight, healthy teeth by sucking and halting the flow of milk.
For information about the best pacifiers check out this post: Why is This the Best Pacifier for Breastfed Baby
Breastfeeding calms your baby down
For newborns, physical, skin-to-skin contact while nursing is crucial. In addition to giving your baby a sense of warmth, security, and comfort, it also increases your body’s production of oxytocin, a hormone that promotes relaxation and facilitates the production of breast milk.
Benefits of breastfeeding for you, mom
New mothers can also benefit from breastfeeding. At the beginning, nursing enables you to immediately sate your baby’s appetite without worrying about bottles, sterilizing bottle nipples, or preparing formula. Also, it can boost your health by reducing your risk of type 2 diabetes, several forms of breast cancer, and ovarian cancer. Breastfeeding can also speed up your uterus’ recovery to pre-pregnancy condition and reduce postpartum hemorrhage.
After giving birth, breastfeeding may also aid in weight loss as your body uses pregnancy-related fat stores for milk production. When nursing, your body burns about 800 calories per day in the first three months of your child’s existence, and then much more in the next three. This is especially beneficial for pregnant women with gestational diabetes who want to regain their pre-pregnancy body weight.
In addition to its health advantages, breastfeeding has long-term financial advantages as well. When your kid develops and needs more food, formula may cost more than $1,500 annually.
Yet, as we previously noted, your breast milk’s nutritional composition varies to meet your baby’s demands, and newborns typically require the same amount of breast milk as they age. Moreover, if you are living in the United States where the healthcare system is private, breastfed infants may experience fewer illnesses, which can reduce the cost of healthcare.

The biology behind breastfeeding
Some of the happiest times you spend with your newborn infant might be while you’re breastfeeding. It allows you to form a deeper connection with your child while providing them with the vital nutrients they need to survive, grow, and stay healthy.
Yet for many first-time mothers, breastfeeding may also be a source of anxiety. Don’t panic if you’re unsure of how to breastfeed successfully or if you’re debating whether to breastfeed or use formula. We’ve compiled all the information you need to decide whether or not to breastfeed, as well as advice on how to make nursing more effective after you have started.
It’s crucial to keep in mind that choosing to breastfeed is a personal decision, and your selection ultimately determines how you will parent your child. Moreover, keep in mind that breastfeeding is a learned skill; when you welcome the newest member of your family, you and your baby will travel this path together.
Breastfeeding: how does it work?
The process of producing breast milk, when it will initially appear, factors that may impact their supply, and how to keep any excess milk their baby doesn’t take are all things that many first-time mothers may wonder about. We’ve addressed a few of the common questions parents have regarding breast milk below.
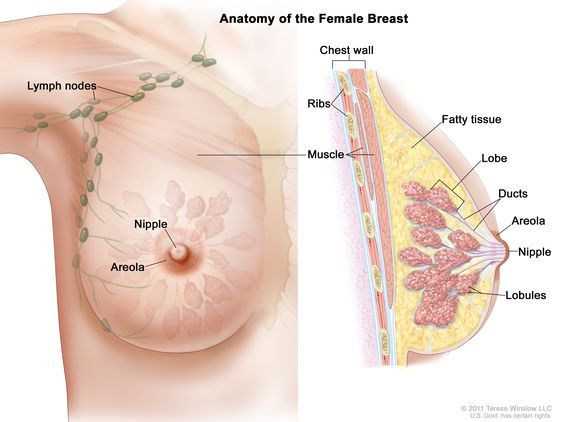
How breastmilk is made
You can better comprehend breastfeeding if you are aware of how your breasts create milk.
Alveoli cells, the areola (the dark region around the nipple), lobes, milk ducts, and the nipple are all constituent elements of the breast. You could see that your breasts enlarge or soften during pregnancy. This is a signal that the alveoli cells, which are located within the lobes of your breasts and make breast milk, are getting ready to go to work.
The hormones prolactin and oxytocin cause the alveolar cells to secrete milk. While your baby suckles, your prolactin and oxytocin levels increase. Your breast contracts as a result of the hormone boost, causing the milk to flow via your milk ducts. SO yes, the more your baby sucks the more milk you will produce, this is why it is important for some moms to buy a milk pump.
The “let-down reflex” is brought on by the flow of milk through your breasts. As your infant starts to nurse, the nerves in your breast transmit signals to your milk ducts to release milk. A few seconds to a few minutes after you start nursing, the let-down reflex might occur, which makes breastfeeding simpler. If you are nursing, it could happen repeatedly.
Let-down can also be brought on by hearing your baby scream or even just thinking about them. Anxiety, discomfort, shame, stress, a cold, too much coffee, smoking, alcohol, and some medicines can all have a detrimental impact on your body’s capacity to initiate the let-down reaction.
When will your breast start producing milk?
Colostrum, transitional milk, and mature milk are the three stages in which your breast milk will be produced. The “liquid gold” known as colostrum is created throughout pregnancy and is there after you give birth. Protein, vitamins, and minerals found in colostrum work together to fortify the body against dangerous germs and viruses. This early milk also helps to prevent jaundice and encourages your baby’s first bowel movement.
Colostrum production from your body will probably be low, but don’t worry—during the early days, your infant just requires a few tablespoons every feeding. When you nurse your baby often, your body will create the next stage of milk within a few days.
The transitional stage is the second stage of breast milk production. After giving birth, transitional milk will start to appear three to four days later. It will resemble orange juice combined with milk and will have less protein and immunoglobulins than colostrum. Transitional milk, however, has a higher lactose, lipid, and calorie content.
Your body will start producing mature milk, which is thin, white, and occasionally somewhat blue in color, between 10 days and two weeks following birth. All of the fat and other nutrients your baby needs to thrive are there in plenty in your mature milk.

What can affect your milk supply?
Your body’s capacity to produce breast milk can be influenced by two main factors:
- How much milk is removed from your body each time you breastfeed. When your breasts are empty, more milk is produced. Milk supply diminishes if your breasts store too much milk between feedings.
- How frequently you breastfeed or pump to eliminate milk. Frequent feeding or pumping increases milk production.
Ineffective latching, using formula in addition to nursing, using certain drugs, preterm delivery, maternal obesity, pregnancy-related high blood pressure, and poorly managed insulin-dependent diabetes are other factors that might result in reduced milk production. Your milk production may also be affected by prior breast operations.
The fundamental rule of thumb is to feed often and thoroughly empty your breasts each time to guarantee adequate milk production. Following feedings, you can try the following techniques to help your infant better empty your breasts:
- Compression and massage of the breast
- During breastfeeding, give your infant both breasts.
- Following breastfeeding, using a breast pump as stated in our post about the essentials of breastfeeding.
You may increase milk production by using a breast pump each time you miss a breastfeeding session, delaying the introduction of pacifiers for your newborn until three to four weeks after birth, and reducing your alcohol and nicotine intake.
What to do before your baby is born?
There are a few things you can do in advance of giving birth to your child that will help you be ready and make nursing easier once your child is here.
- Invest in prenatal care, which includes visiting prenatal checks and selecting a doctor to oversee your pregnancy. This might prevent a preterm delivery for you (babies born before 37 weeks of pregnancy). Breastfeeding difficulties are more common in premature newborns than in full-term infants.
- Attend a breastfeeding class to learn the fundamentals. Some organizations and hospitals offer breastfeeding programs.
- Speak with Your Doctor and discuss your desire to breastfeed with your physician to determine whether any past wounds you may have sustained or any vitamins, drugs, or birth control you may be on are safe to breastfeed while taking. Your doctor may also make sure you can nurse your infant as soon as possible after birth, which is crucial for the first hour of the child’s life.
- Speak to mommy friends or join a breastfeeding support group. If you have any questions, they can answer them and give help in a safe space, sometimes you may feel shy in hospitals.
- Purchase everything you need. You can learn about the essentials of breastfeeding in our post.
Breastfeeding on practice
After discussing the advantages of breastfeeding and how it functions, it’s time to discuss how you nurse your child. Whether you’re a first-time parent or have given birth more than once, you’re likely to find some advice on how to make nursing less difficult and more enjoyable for both you and your child.
How long should breastfeeding last?
Since there is no prescribed duration for feedings, many mothers seek information to understand how much milk their infants should consume.
Despite the fact that feeding sessions might run anywhere from 15 to 45 minutes, your baby will eventually let you know when they are done. In the early days or during growth spurts, your baby may take longer or less time and require more feedings. The trick is keeping an eye out for your baby’s cues that they’ve had enough.
As your infant releases the nipple, keep an eye on him or her and stop feeding. If your infant won’t let go, stop feeding after the cycle of sucking and swallowing slows down to around four suckings for every one swallow. When your baby’s hands are no longer clenched in a boob and they seem tired and calm, you’ll also know that they’ve had enough. Burp your infant and switch to the other side after they’ve done from your initial breast. You can feed him or her till the second breast, where they cease.

How often should I breastfeed?
You should start breastfeeding as soon as you can after giving birth since it is very important for your baby during these first few hours.
After giving birth, you should nurse your baby eight to twelve times in a 24-hour period, or around every two to three hours. You might need to feed your baby every one to two hours in the first few days after delivery. As a result, your body will make adequate milk and your baby will eat enough.
It’s crucial to remember that every infant has different feeding habits. You can wait an hour between feedings if your infant is more ravenous or eager, as opposed to three hours if they are more readily satiated.
Instead of feeding your kid on a schedule, it is ideal to feed them when needed. Keep an eye out for signs of hunger in your baby, such as increased alertness or activity, mouthing, rooting, and sucking. Even though crying is a symptom of hunger, it’s sometimes a late indicator for your infant. This can make it more challenging to breastfeed.
It’s possible that your newborn’s appetite won’t start to develop until three days following birth. To ensure your kid gets adequate nutrition in the early days if there isn’t a demand for feedings from them, you might have to begin or urge them to feed. Your pediatrician may suggest that you wake your baby for feedings every three hours if they are particularly drowsy.
Your infant may desire to “cluster feed” in the beginning, which is to feed numerous times quickly followed by an extended period without feeding. Every hour or multiple times in an hour, particularly in the evening and at night, your infant may nurse. Anytime during the day, your baby should feel full after a cluster of feedings.
How do I know when my baby is hungry?
Science believes that it’s best to feed on demand when your baby is hungry. At the end, our body is smart and it knows what it needs. However, since the babies don’t talk, it is hard sometimes to know when a baby is full. Here are some signs to detect if your baby is hungry:
- Nuzzling against your breast
- Opening their mouth
- Sucking furiously on their hand, shirt or even your arm
- Rooting reflex
- Smacking their lips
- Hungry sound as learned in the “what is your baby saying” post

How do I know if my baby is getting enough?
The belly of your baby will be extremely tiny, especially in the early days.
Babies who are breastfed and between the ages of 1-6 months often consume 19 to 30 ounces of breastmilk per day. If your infant eats eight times each day, this works out to 3 ounces every feeding. But remember that every infant is unique. Your newborn’s stomach can safely absorb one to two tablespoons of milk at birth. Their stomach will have expanded by day 10 to accommodate around two ounces of milk.
Your kid will typically grow up to 1 ounce of weight every day from birth until age 3 months. Yet, up to 7–10% of your baby’s birth weight might be lost in the first few days. Gaining 4 to 7 ounces per week after the second week is common. At your child’s initial appointments, your physician will keep track of your child’s weight.
Knowing if you’re making enough milk and if your kid is eating enough might be difficult. You may keep an eye on a few markers, the first of which is your infant’s bowel motions.
If your baby has frequent bowel movements, you will be able to tell if he or she is getting enough milk. In the first five days, the color of newborn feces normally changes from black to brown to mustard-yellow. Your newborn should have at least two to three bowel movements in a 24-hour period by the third day after delivery. At the age of five days, your infant could pass at least four seedy, yellow stools each day. As your baby gets older, the frequency of bowel movements will change, with some babies having one every day and others having one every few days.
Your baby’s dirty diaper can also serve as an indicator as to whether they are getting enough to eat or not. From these 3 you should expect from 5 to 7 diaper changes, if it’s more or less by far and for more than 3 days you should go to your doctor.
- Some indications that your infant is eating enough include:
- Instead of being dark yellow or orange, your baby’s pee is pale.
- Your baby may be heard gulping down the milk.
- After feeding, your baby is content and comfortable.
- After nursing, your breasts feel softer.
- Your infant alternates between brief naps and attentive, awake times.
At what age should I stop breastfeeding my kid?
The American Academy of Pediatrics (AAP) advises nursing your infant for the first six months exclusively with breastmilk. You may start feeding your baby solid meals along with breast milk at six months of age. The AAP further advises continuing to nurse your child beyond their first birthday and for as long as you and your baby both desire.
Despite the fact that nursing for as long as feasible has many benefits, only 57.3% of mothers nurse their infants for the advised six months, and only 36.2% continue to do so for a full year.
When your kid initiates the process, it will be the simplest to wean your child off of breastfeeding. But you should also choose nursing strategies that fit your needs and way of life. Returning to the workforce, improving your health, or simply feeling that the time is right may be the driving forces behind your choice to quit nursing. In the end, it’s up to you.
Also notice that Pacifiers can serve as a helpful tool during transitions from breastfeeding to bottle feeding or introducing solid foods. They provide familiarity and can ease the process of adapting to different feeding methods. For more information on pacifiers and which one to choose check out our post about pacifiers for breastfed babies: Why is This the Best Pacifier for Breastfed Baby

Are there times when breastfeeding is not recommended?
The best course of action is to speak with your doctor before nursing if you take frequent medication or are ill.
It is usually advisable to verify, but medications that are safe to use during pregnancy are normally also safe to take during nursing. If your infant exhibits any symptoms of a response to your breast milk, such as diarrhea, excessive crying, or tiredness, you should also see a doctor.
It’s normal to worry about breastfeeding when you’re feeling under the weather, but you can typically continue to nurse even when you or your baby are ill. It’s always OK to pump or manually express breast milk for someone else to give the infant a bottle if you need more rest.
Allowing your baby to start looking for your breast to feed on is one way to get them to latch. This method of nursing, known as “baby-led breastfeeding,” allows your infant to take the initiative and follow his or her innate need to suck.
Here are a few techniques to encourage your baby’s relaxation and a natural latch:
- Relaxing on cushions or in another cozy spot might help you create a peaceful atmosphere.
- Before nursing, unwind and hold your child skin-to-skin between your breasts.
- Allowing your baby to take the lead when they are hungry. Your infant may bob their head against you, make an effort to look at you, or move around.
- While your infant reaches for your breast, support his or her head and shoulders.
- Letting your breast dangle naturally so that your baby may obtain a full mouthful as their chin rests on your breast
In the event that the baby-led method does not result in a successful latch, try tickling your baby’s lips with your nipple to get them to open their mouths, pulling your baby close so that their chin and lower jaw move into your breast, or aiming your baby’s lower lip as far away from the base of the nipple as possible to get them to take a big mouthful of breast.
Breastfeeding should not be painful
During nursing, your breasts are your greatest asset. Yet you can encounter some difficulties if they are working overtime. Many typical factors for nipple discomfort while breastfeeding might include:
- Mastitis. The infection that enters the breast is what is causing this breast inflammation. It produces flu-like symptoms as well as red irritation and breast tenderness. When bacteria enter a milk duct through nipple fissures, mastitis frequently results. Engorgement can be avoided by pumping or breastfeeding your infant. Breastfeeding relieves an illness if it develops, and it is safe to carry on. In order to get rid of the illness, your doctor will also prescribe an antibiotic.
- Milk ducts blocked. You can have a clogged duct if you see a painful, inflamed area on your breast. Continue nursing in hopes that the obstruction will ultimately dissolve. Blockage can also be relieved with a warm compress.
- Cracked or sore nipples. It’s not necessary for your breasts to feel painful just because they’re working harder than usual. Make sure your infant has a healthy latch by adjusting your nursing posture. In addition, there are some products that can help you with these cracked nipples as you can see in our post about essentials for breastfeeding.
Latching
The way a baby takes the breast into their mouth to feed is called the breastfeeding latch, and it is very important. A good breastfeeding latch means your baby will be able to remove the milk from your breasts efficiently, which should keep your milk supply steady and plentiful. It also helps you avoid sore nipples.
Guiding a newborn to latch correctly may take some trial and error. To latch properly, your baby should be latching onto your entire nipple as well as some of your areola. If their lips are turned outward (like fish lips) and their chin and nose are touching the breast, those are good signs they’ve latched on well.
If you cannot get your baby to attach correctly, there are some other options to help you as you can learn in our post about breastfeeding essentials.
Using formula
Doctors generally agree that breast milk offers the most nutritional value for your baby, but some moms may want to formula-feed their child for a variety of reasons, including comfort, the demands of their lifestyle, or a specific medical condition.
Formula is a good option for mothers who are unable to breastfeed since it may provide their child the nutrition they need to develop and be healthy.
You should only use commercially manufactured formulas since they are made to closely resemble the complex blend of proteins, carbohydrates, fats, and vitamins present in breast milk.
The advantages of formula feeding your child include:
- Convenience: Your infant can take a bottle at any time from either parent or another caregiver (although this is also true for women who pump their breast milk).
- Frequency of feeding: Formula is less digestible than breast milk, thus babies who are fed formula often need to eat less frequently than those who are breastfed.
- Diet – While utilizing formula, you don’t have to be concerned about what you eat or drink.
On the other hand, there are several typical difficulties moms may have during formula-feeding.
- Absence of Antibodies – Unlike breast milk, formulas do not provide your infant any antibodies. The additional defense against disease and infection is removed as a result.
- Preparation is required for formula feeding since you must purchase the formula, prepare it, and keep the bottles and nipples handy for when your baby is hungry. Making formula for your infant requires preparation time and planning, unlike nursing, which may happen whenever.
- Expense – As previously said, formula may be pricey, with a one-year supply costing around $1,500 (in the UE). Formulas in powder form are frequently less expensive than concentrated, ready-to-feed formulas. The most costly formulae are often those designed specifically for infants with specific allergies or intolerances.

What to eat while breastfeeding
It’s common to question whether the food and beverages you consume while nursing will have an impact on your breast milk and, in turn, your kid. Fortunately, for the majority of women, only a small number of foods should be avoided during nursing because of the potential harm they may cause to your child; otherwise, anything goes. Better still, a lot of foods can increase your milk production!
We’ll go through the things you might want to add to your diet as well as those you might want to cut back on until your child quits nursing.
Foods that can increase your milk production
Certain meals, referred to as lactogenic foods, can boost both the quantity and nutritious content of the breast milk your body produces.
You don’t want to consume too many lactogenic foods, just like you shouldn’t with any other aspect of your diet. Breast engorgement, blocked milk ducts, and mastitis are just a few problems that can result from excessive breast milk production.
Yet, including some of these regular items in your diet may benefit both you and your unborn child. SOme of the most known lactogenic foods are:
- Fennel and Fenugreek Seeds
- Leafy Greens and Reddish Vegetables
- Barley and Barley Malt
- Oats
- Garlic and Spices
- Brewer’s Yeast
- Spirulina
- Healthy Oils and Fats
Foods to limit while breastfeeding
There are very few foods you need to eliminate from your diet while breastfeeding. However, there are a few things you should limit, such as alcohol and caffeine, that can impact your baby’s health and your milk supply when consumed in large quantities.
- Alcohol: Two alcoholic drinks per week are often seen as safe when nursing. Alcohol can get into breast milk, although it normally only does so in very minute levels. However, it is a must if you wait to start drinking again when your kid has stopped breastfeeding.
- Caffeine: An excessive amount of caffeine might irritate and overstimulate your baby. The recommended daily limit for caffeine consumption is three. Caffeine, like alcohol, may cross into breast milk, therefore it’s best to avoid consuming it while breastfeeding.
- Fish: During nursing, it’s best to stay away from fish that are known to have high amounts of mercury, such as shark, swordfish, tilefish, and king mackerel. The advantages of eating other kinds of fish often exceed any hazards since they have mercury levels that are minimal enough. It is okay to consume 12 ounces of low-mercury seafood per week, such as shrimp, salmon, pollock, or catfish.
- Chocolate: An excessive amount of chocolate might irritate and overstimulate your kid.
- Herbs: When it comes to nursing, peppermint, parsley, and sage often have a poor image since some mothers think they might reduce milk supply. But, for these three herbs to have an impact on you or your unborn child, you would need to eat them in extremely high doses. It is okay to use them to season or flavor meals.
If you discover your infant is badly impacted by certain foods, such as soy, dairy products manufactured from cow’s milk, gluten, eggs, peanuts/tree nuts, and citrus, you may need to exclude them from your diet. These foods are the main causes of several widespread food intolerances. Just omitting one of these items from your diet should address any concerns if you detect a negative reaction in your kid (such as gastrointestinal problems or irritability) after eating it.

Which Medications Are Safe to Take While Breastfeeding?
The majority of medications that are in your blood can pass into breast milk. Nevertheless, most drugs only concentrate in breast milk at very low concentrations that are completely safe for your infant. Before starting to breastfeed, it’s advisable to discuss the drugs you’re taking with your doctor as well as any potential hazards or concerns.
There are several drugs that should not be used while nursing, even when the benefits of doing so, particularly for chronic diseases, exceed any possible hazards. When the medicine is present in your breast milk at low levels, your doctor may advise nursing or alternate treatments in these situations.
While using certain drugs, your doctor may occasionally advise you to discontinue nursing temporarily or permanently. If you know in advance when you won’t be able to breastfeed, you can pump in addition to feedings and save milk for later use.
Medications that are safe
The following medicines are thought to be safe to use while nursing, according to the Mayo Clinic. This is not an exhaustive list of all drugs that are safe but rather the most commonly used ones.
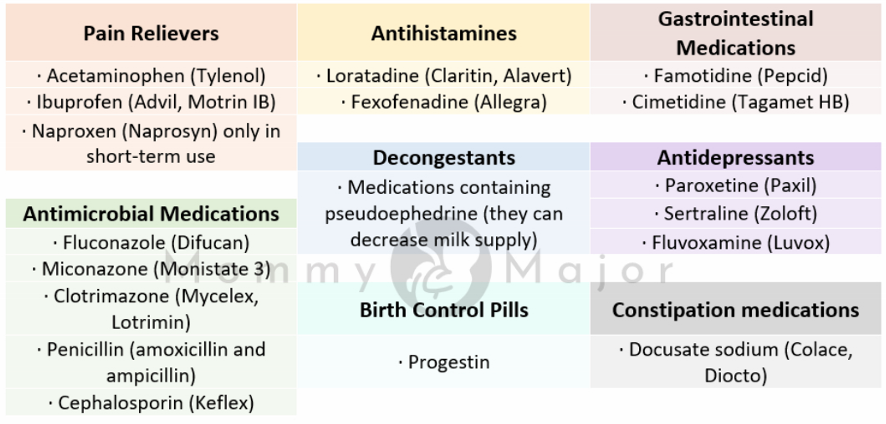
Some medications that your doctor may advise you to stop taking while breastfeeding include:
- Bromocriptine (parlodel) to treat Parkinson’s disease
- Chemotherapy drugs
- Ergotamine for migraine headaches
- Lithium for manic-depressive illnesses
- Methotrexate for arthritis
- Nicotine
- Abused substances such as cocaine, PCPC, amphetamines, heroin and marijuana
However, it is very important for your baby’s safety to talk to your doctor and to be very clear about everything you are doing, eating and consuming.
Explore other Topics
The best books for pregnancy, reading only one booked we have seen that the confidence of the mother in herself and the process is highly increased. Whether you’re looking for practical advice, emotional support, or simply an enjoyable read to help you relax, this list has got you covered. So grab a cup of tea, curl up on the couch, and explore the best pregnancy books of 2023.






